On this day in 2018, our lives were forever changed, for the better! We didn’t start the blog until the girls were a couple months old, so let’s flashback to hospital bed rest and Delivery Day!
14 Week Ultrasound
I think back to the last few weeks before babies a year ago, how I was SO ready to not be pregnant anymore, with the swollen feet, smooshed stomach thanks to Emerie, crushed bladder courtesy of Harper, and crunched rib cage thanks to Reagan, and wonder how I made it through!
If I had to pick a toughest week during the pregnancy (ignoring the 4 months of solid “morning” sickness that lasted every second of the day), it would be Week 30. I actually felt better Week 31 and 32. We measured the belly on the weekend of that brutal week, and I grew 5″!! Granted some of that was probably the girls shifting around a little, but FIVE INCHES. Not enjoyable and no amount of repositioning made me feel comfortable.

Big belly the day before they arrived!
Much of my one-day of hospital bed rest is a blur and I wish I had written it down! I do remember I could not get comfortable in the bed, even with a ton of pillows, and had a really hard time getting up to go pee! My hip joints were excited at the prospect of baby delivery, with my left side hurting more than my right.
Once admitted, the nurses worked to get an IV line in my arm. My veins did not cooperate and looking back, it’s pretty funny (not so much at the time). Providence has a two stick rule, so after three nurses gave my IV a shot (a “shot”, get it haha) and failed, one of the anesthesiologists was called. Like a rock star, she was able to access the vein in my left hand on the first try and did it so fast, I was bleeding on the floor.

A beautiful day for triplets!
I started hospital bed rest at 32 Weeks+6 Days gestation and was very happy to have stalled that long before being admitted. Dr. Ritchie knew and understood my concern on staying in the hospital, and agreed to closely monitor but allow me to stay home from January to March, where I spent my time working from the recliner and helping the girls cook a little longer. I believe they stayed in longer because I was at home, in my comfort space, and not uncomfortable and confined to a hospital room. There are many expecting moms in my Facebook group that handled extended hospital stays so well and I really applaud them.

I did a 24 hour urine test, which ultimately determined the babies’ arrival. The test returned with high levels of protein, signifying kidney function issues. My blood pressure also indicated pre-eclampsia may be an issue. Dr. Richey gave me the choice of a March 20th or March 21st birthday, and I chose a soon as possible. In retrospect, if given the chance again, I would pick the latter, because my breakfast order was canceled with the surgery scheduling. It was a LONG day full of nerves and starvation. Ice chips can only help for so long!

Birth Plan!
Scheduling the C-section took about eight hours- Dr. Richey had to call in staff to ensure enough nurses and doctors were available to handle three 33 weekers plus me! Each baby required a nurse as well as a few others. The dad even gets his own support nurse during surgery. I also needed an anesthesiologist and several doctors.
It was quite the party! It really surprised me how quickly that time passed. In total, I was only in the operating room for maybe an hour, and I walked myself in there and sat down on the operating table for the spinal block. It wasn’t as bad as I expected and felt like a warm rush of water drifted down my legs. Before I even realized it I was on the table, ready for go-time. Simultaneously, Craig was out in the pre-op area getting on his gown so he could come in.
My support person while Craig tended to babies!

About to be go-time!
What I found out later was the planned C-section became emergent the moment I received the spinal. Doctors are used to handling pressure and gave no indication anything was wrong, just that everything was getting ready for go-time. What I was told later was that Baby B’s (Emerie) heart rate significantly dropped into the 40s, and there was no time to wait.
Dr. Richey asked “can you feel this?” to which I responded no, and within seconds the first of three, Baby A, was born. Instantly I felt a huge relief of pressure. It is hard to explain, because everything was numbed, but I could tell when each was born. We requested prior to surgery that the girls come out in the A, B, C order we had grown accustomed to and tracked throughout the pregnancy, knowing they would be referred to that until they received real names. Conveniently at this point, Baby A was in the middle (bladder baby), Baby B on my left side, and Baby C nestled on the right, so the order worked perfectly. With B’s heartrate dropping dangerously low, A was pulled out with the cord still connected while B was born.
Looking back, it makes sense that little Emerie would want to make an entrance, while Harper and Reagan patiently waited for their sister to get attention. By the time Craig made it into the OR, Emerie was already out and almost headed down the hall toward the NICU. There was a bit of commotion, as Dr. Richey ensured the nurses knew this was Baby B, NOT A, even though she was the first out of the room. Baby A followed a few moments later and then Baby C. Craig was able to see Harper and Emerie as they were whisked away to the NICU for assessment. Dr. Richey surprised me with a view of a screaming Baby C (Reagan), freshly born over the curtain, before she headed off to the NICU.
We joked much of the pregnancy that if a fourth baby was hiding out in there, Dr. Richey would be taking them home, unless it was a boy, then they’d get A, B, or C. Luckily, she had correctly counted three girls all along. Baby A, Harper Anne, was officially born at 4:58 PM, with Baby B, Emerie Faye, about 30 seconds behind her, and Baby C, Reagan Jean, at 4:59. No one officially received a name until we saw them in the NICU; and it turned out pretty great that the order spelled out “HER”. That was not pre-planned!
Craig headed off to the NICU with the babies as planned, and I was stitched up and moved into recovery. At this point my high blood pressure indicated eclampsia was an issue. My memory is a bit blurry here, but I do remember that I was arguing against a magnesium drip and on the line of getting it whether I wanted to or not. My blood pressure was checked every five minutes and took over an hour to come down. I didn’t get to see the girls until about 8 PM, partially due to shift change and partially due to my blood pressure issues.
I spent more time in post-op recovery than the actual surgery and ended up staying in the hospital a few more days that originally planned. When Emerie’s heart rate plummeted, Dr. Richey immediately sliced, once I agreed I felt nothing, to get to her. This meant I did not receive the full cleaning beforehand, which opened me up (pun intended!) to a higher risk of infection. I was given an antibiotic drip that took 1.5 hours to administer, a handful of times per day, for five days. Between that, pumping and spending time in the NICU, things were pretty hectic.
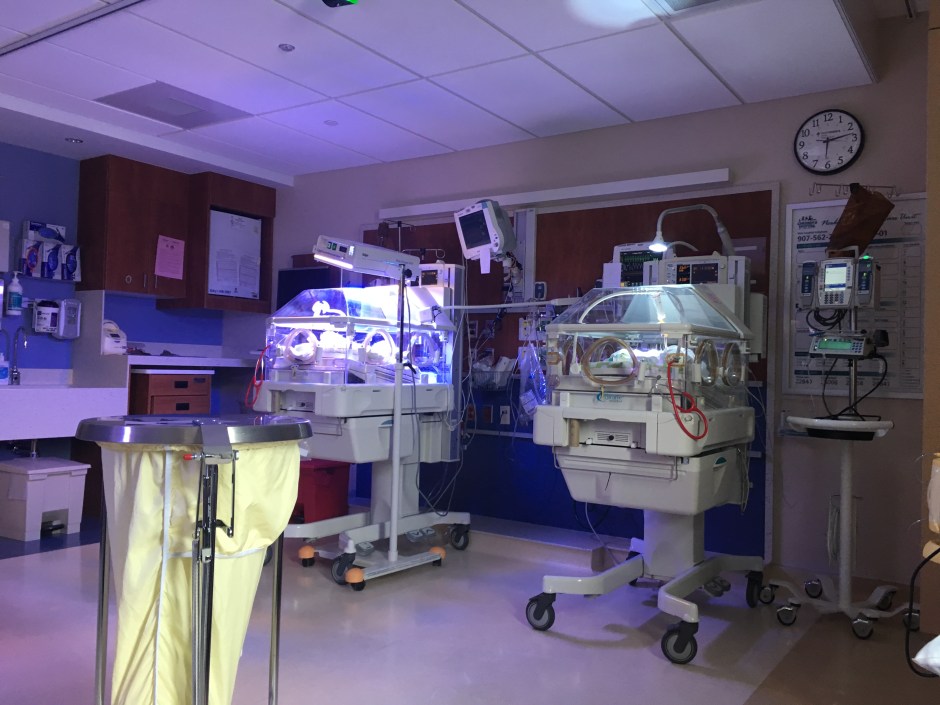
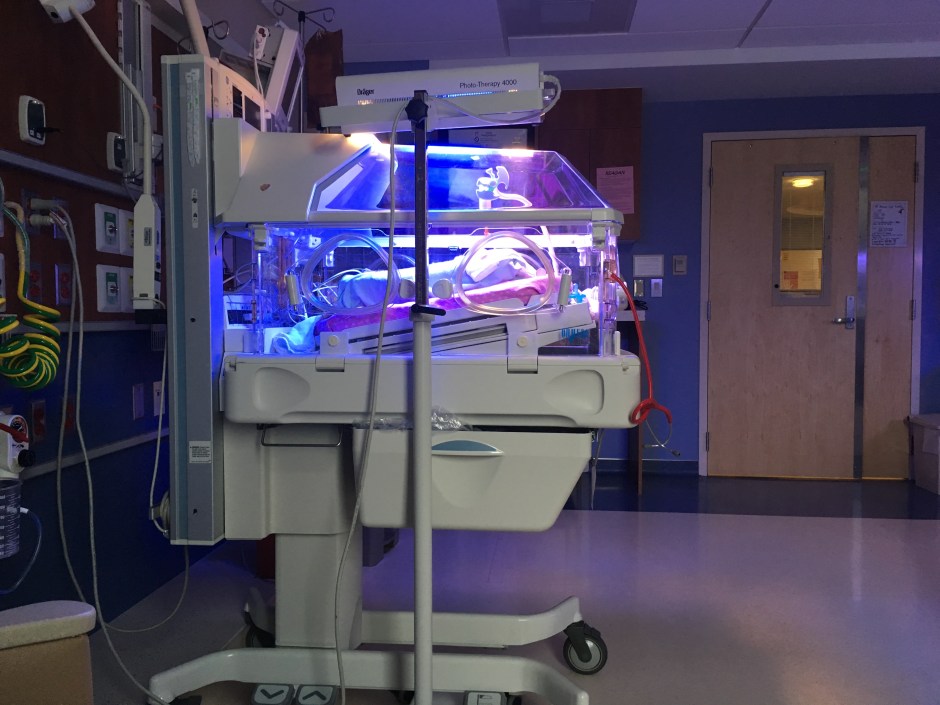
What a relief to have made it to my goal of 33 weeks gestation! At that mark, the risk of brain bleeds goes down over 90%. The girls all briefly had CPAP air as well as jaundice lights, but overall came out incredibly healthy and good sizes for their age.
Harper Anne Douglas: 4 pounds, 8 ounces, 17.9” long 
Emerie Faye Douglas: 3 pounds, 2 ounces, 15.3” long
Reagan Jean Douglas: 4 pounds, 5 ounces, 17.7” long
How has it been a year since they arrived?!

The girls at about 6 Weeks, taken by Alaska Photography & Design




















